Why Telijie Disposable Babys’ Bibs Are a Parent’s Best Friend
1. Soft & Skin-Friendly Material – Gentle on Delicate Skin
Crafted with a 3-layer design using premium spunlace non-woven and waterproof PE film, our bibs are ultra-soft and lint-free. They feel gentle against your baby’s sensitive skin, with no harsh chemicals, scratchy edges, or irritating textures. The lightweight fabric keeps your child comfortable during long meals, snacks, or even messy craft time, without weighing them down or causing discomfort.

2. Superior Mess & Stain Protection – No More Laundry Nightmares
The top absorbent layer quickly soaks up liquids like milk, juice, and soup, while the waterproof backing creates a leak-proof barrier to stop food, sauces, and spills from seeping through to clothes. The deep, integrated food pocket catches crumbs, dropped bites, and drips before they hit the floor or your child’s outfit, keeping mealtime mess contained in one easy-to-dispose bib. No more scrubbing stubborn food stains off multiple bibs or outfits every night!
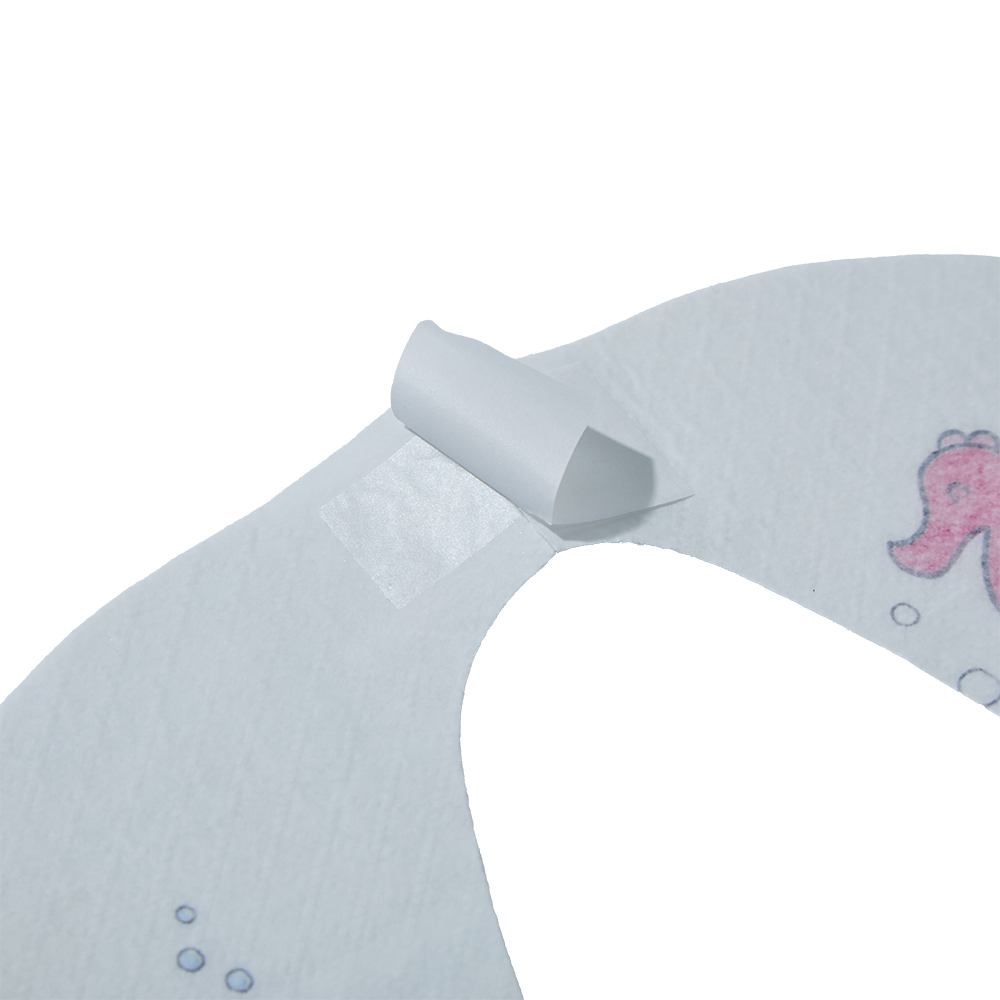
3. Fun, Kid-Friendly Design – Comfortable & Convenient to Use
Our disposable kids’ bibs feature an adjustable, tear-resistant neck closure that fits babies and toddlers of all sizes, from infants to preschoolers. The flexible closure is easy to fasten and remove with one hand, perfect for busy parents juggling mealtime chaos. Lightweight and compact, they fold flat to fit in diaper bags, purses, or stroller pockets, making them ideal for restaurants, travel, daycares, and on-the-go meals. Plus, they come in cute, playful prints kids love!

4. Hygienic & Single-Use – Safe for Every Little One
Designed for one-time use, our disposable bibs eliminate the risk of cross-contamination and bacterial buildup that comes with reusable bibs. Each bib is fresh, clean, and ready to use right out of the package, making them a safe choice for daycare centers, playdates, or when sharing meals with friends. Manufactured in dust-free facilities with strict quality control, they meet global safety standards for children’s hygiene products, so you can rest easy knowing your little one is protected.

Who Are These Bibs Perfect For?
-
Busy parents of babies, toddlers, and young kids
-
Daycare centers, preschools, and nurseries
-
Restaurants and family-friendly cafes
-
Traveling families and road trips
-
Daycares and babysitters looking for low-hassle hygiene solutions
Ready to Make Mealtimes Stress-Free?
Telijie Disposable Kids’ Bibs are more than just a mealtime accessory—they’re a simple way to keep your child clean, comfortable, and happy while cutting down on cleanup time. Whether you’re stocking up for home use, daycare facilities, or retail distribution, we offer flexible bulk orders and custom printing options to suit your needs.
Contact Telijie Sanitary Materials Co., Ltd. today to request samples, explore pricing, or learn more about our range of children’s hygiene products!